After a period of time trying for a baby with your partner without success, you may be thinking about going for a fertility study.
Fertility tests are fundamental when a couple has been maintaining unprotected sexual relations for more than a year without getting pregnant. The causes of infertility can originate from the female, the male, or a combination of both.
For women, a fertility study consists of a series of tests, among which is a hormonal analysis and an ultrasound. In this article, we discuss what the female fertility study entails and explain each of the tests that are involved.
FEMALE FERTILITY TESTS
The first step is for the woman to visit her gynaecologist. The gynaecologist will evaluate her general state of health, her personal and family medical history, as well as other factors that can influence fertility such as lifestyle habits and diet. In this way the patients clinical history can be studied to indicate which fertility tests should be performed.
The main fertility tests for the female fertility study are as follows:
- Transvaginal ultrasound and pap smear
- Hormonal Analysis
- Hysterosalpingography (HSG)
- Karyotype study
- Hysteroscopy (HSC)
- Endometrial biopsy
TRANSVAGINAL ULTRASOUND AND SMEAR TEST
The first test in the female fertility study consists of an examination of the female reproductive apparatus. This is done by a transvaginal ultrasound to analyse the condition of the vagina, uterus and functioning of the ovaries. This test allows us to perform an antral follicle count when done in the first few days of the menstrual cycle, to be able to evaluate the ovarian reserve. It is also advisable to have a smear test to rule out any possible infections or injuries to the vaginal cells and cervix.
HORMONAL ANALYSIS
Hormonal imbalances can also affect the menstrual cycle, resulting in female infertility. To make sure there are no problems, the following hormones are studied in women:
- Follicle stimulating hormone (FSH): is a gonadotropin released by the pituitary gland that can be used to estimate the ovarian reserve. The normal range is between 3 and 9 mUI/ml, whilst values above 13 – 15m mUI/ml are a sign of a poor reproductive prognosis.
- Luteinising hormone (LH): also produced by the pituitary and gives us information about how the ovaries are functioning and ovulation. At the start of the cycle, the level in the blood should be between 2 and 10 mUI/ml.
- Progesterone: is secreted by the ovaries after ovulation and permits us to know if the egg has been released or if there are ovulation problems. Around day 21 of the menstrual cycle, the levels should be greater than 5 – 10 ng/ml.
- Estradiol: produced by the ovaries and is used to evaluate follicle development, the endometrium and the ovarian reserve. If levels are found to be above 100 pg/ml, it could indicated reproductive problems.
- Anti-Müllerian hormone (AMH): released by the ovarian follicles, its levels are proportional to the number of eggs in the ovaries. A good ovarian reserve is indicated by values between 0.7 and 3.5 ng/ml, whilst values lower than 0.7 ng/ml signal that menopause is near.
According to specialists, when female fertility tests are performed, the most common is to do the hormonal analysis between days 2 and 5 of the menstrual cycle. The only exception to this is progesterone, the study of which should be done around day 21 of the cycle to check if ovulation has occurred.
HYSTEROSALPINGOGRAPHY (HSG)
Another test used in female fertility testing is the hysterosalpingography (HSG) in which the structure of the uterus is studied using X-rays. Furthermore, it enables the specialist to know if the Fallopian tubes are permeable, which is important as this is where the egg and sperm meet to fuse and form the embryo. If the Fallopian tubes are obstructed, it will be necessary to opt for in vitro fertilisation (IVF) to achieve the pregnancy.
KARYOTYPE STUDY
This fertility study is used to detect possible abnormalities in the number and structure of the chromosomes, which can cause infertility in the woman. It is done via a blood test to look at the white blood cells, or lymphocytes.
This study is recommended in the event of repeated miscarriages and implantation failure.
HYSTEROSCOPY (HSC)
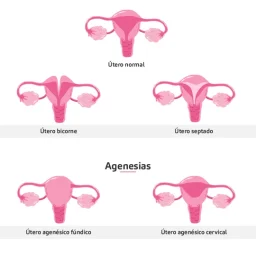
This is a fertility test, which, with the aid of a hysterocope (a thin tube containing a camera), can diagnose abnormalities in the uterus and endometrium, such as polyps and fibroids.
This fertility study can allows us to determine the reason why pregnancy has not occurred, and is especially recommended in cases of miscarriage and before starting any fertility treatment.
ENDOMETRIAL BIOPSY
The endometrial biopsy is a study which consists in taking a sample of the endometrial tissue, using a biopsy catheter, so that the specialist doctor can analyse it and check for any anomalies at the cellular level.
This female fertility test is sometimes recommended in cases of implantation failure to check for endometrial receptivity.
Now you know what a female fertility study entails and, if you wish to become pregnant, at our Ovoclinic assisted reproduction clinics we can help you to achieve it.